Parents often arrive in my clinic saying, “I think my lip tie baby can’t latch,” or “Someone told me we need a laser release.” The internet is full of dramatic photos and confident promises, but medicine asks for something more careful: function over appearance, and relief over hype. In this long, practical guide, I’ll explain what a lip tie is, what really matters during feeding, when procedures help, when they don’t, and how I personally evaluate and support families. You’ll also see exactly how I fold research, clinical reasoning, and compassionate counseling into a step-by-step plan for a lip tie baby—without shortcuts, and without pressure.
Table of Contents
What Is a Lip Tie (and Why the Name Confuses Families)?
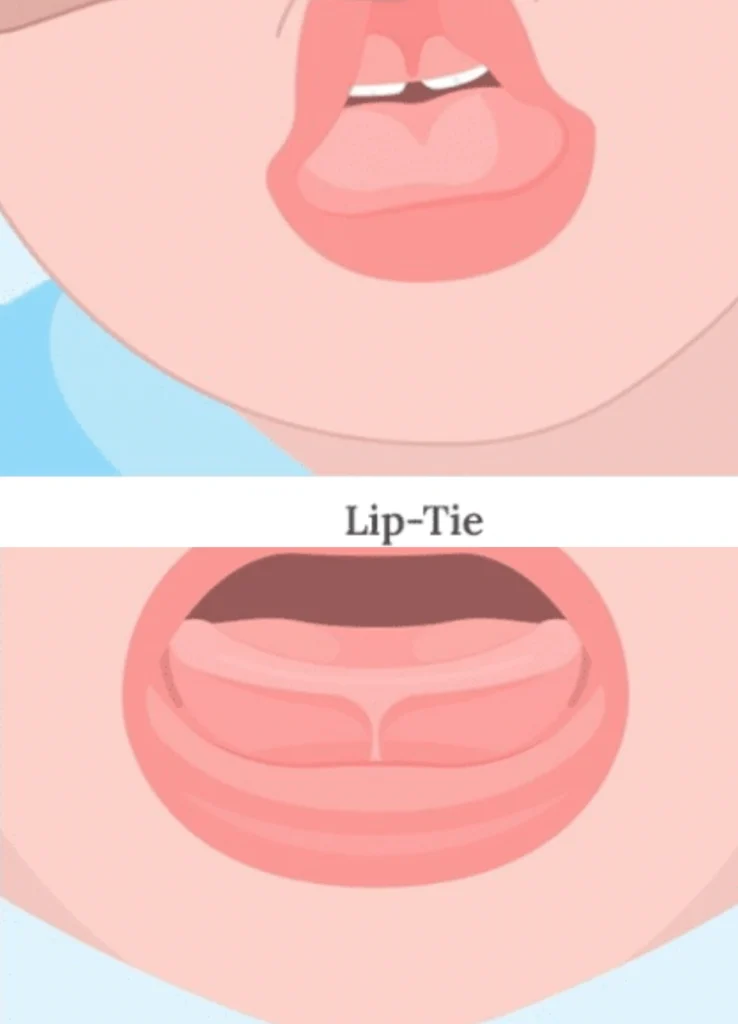
A lip tie is a description of the maxillary labial frenulum—the small band of tissue between the upper lip and the gum—when it appears tight, inserts low near the gum line, or seems to restrict how the lip flips upward during a latch. Every baby has a frenulum; variation is normal.
The problem isn’t the presence of the tissue, but whether it creates a functional restriction for your lip tie baby during feeding. Parents are often shown grades or scales based on where the frenulum inserts. Those grades describe appearance, but appearance alone doesn’t decide if feeding will succeed. Many thriving babies have a prominent frenulum, while some struggling babies have a normal-looking one. That’s why the smartest first step for a lip tie baby is not a photo, but a careful observation of a real feed.
Key idea: anatomy matters, but function rules. For a lip tie baby, the decision to treat or not to treat must be driven by latch quality, milk transfer, comfort, and growth—not by a number or a snapshot.
Lip Tie vs. Tongue Tie: Why People Mix Them Up
Tongue tie (ankyloglossia) refers to a tight lingual frenulum that limits tongue elevation or extension. Research on tongue tie and breastfeeding is broader than the research on lip ties, but even there, the data are mixed. Sometimes a lip tie baby also has a suspected tongue tie, and symptoms overlap: shallow latch, clicking sounds during feeds, prolonged feeding sessions, nipple pain, gassiness, or slow weight gain.
Because both structures sit in the same small space and both affect latch mechanics, families naturally ask whether both need release. In practice, many feeding issues improve with skilled lactation support even when a frenulum looks tight. The lesson for a lip tie baby is simple: test function with hands-on help before assuming that tissue is the main cause.
How I Evaluate a Lip Tie Baby in Clinic (My Doctor’s Process)
When I meet a lip tie baby, I slow down and build a plan in five deliberate steps:
- History and goals. I listen first. Are the feeds painful? How long do they last? What positions have you tried? Is your priority exclusive breastfeeding, pumping, combination feeding, or comfortable bottle feeds? Your goals set the direction for care.
- Observation of a full feed. I watch an entire breast or bottle feed because real-time function matters more than a still image. For a lip tie baby, I look at how the upper lip flanges, how the tongue elevates and cups, whether the jaw moves smoothly, and whether swallows are rhythmic. A good latch looks deep and asymmetric, with more areola below the nipple than above, and the upper lip usually everts gently without excessive pressure on the gum.
- Oral exam in context. I check the palate shape, tongue elevation and lateralization, the elasticity of the upper lip, and the exact site of frenulum insertion. Importantly, I evaluate elasticity, not just appearance. If the upper lip can comfortably flip without blanching the tissue, a lip tie baby may have normal function even if the frenulum looks “thick.”
- Targeted conservative changes. Small adjustments do big things. Laid-back positioning lets gravity help the baby achieve a deeper latch. Side-lying can reduce maternal tension. Brief hand expression before latch can coordinate let-down with the baby’s rhythm. For bottle feeding, paced techniques and appropriate nipple flow often resolve aerophagia and gas in a lip tie baby without any procedure.
- Follow-up with data. I ask for weight checks, diaper counts, and a pain score. If both baby and parent are improving, no procedure is needed. If there is persistent poor transfer, persistent high pain despite optimal technique, or faltering growth, we discuss next steps in a calm, shared-decision approach.
This method respects science, protects families from unnecessary procedures, and—most importantly—gets relief. Many lip tie baby cases improve dramatically within 48–72 hours when latch and milk flow are optimized.
Signs to Watch in a Lip Tie Baby (Function, Not Fear)
A lip tie baby deserves a thoughtful assessment when you see:
- Shallow latch or frequent slipping off the breast or bottle
- Clicking sounds, prolonged feeds, or milk leaking from the corners of the mouth
- Maternal nipple pain, cracks, or bleeding after attempting better positioning
- Poor weight gain or a pattern suggesting low milk transfer
- Significant gassiness or fussiness tied to aerophagia during feeds
Each sign is a clue, not a verdict. Plenty of babies display one or two of these issues for reasons unrelated to a frenulum—such as a fast let-down, a sleepy newborn pattern, a bottle nipple that’s too fast, or simple early-weeks coordination challenges. The right question is: does your lip tie baby improve with expert feeding support? If yes, a procedure may not be necessary.
What Parents Are Told Online vs. What We Actually See
Online communities often present a binary: “release or fail.” In reality, there is a productive middle ground. In clinic, I routinely meet a lip tie baby whose family has been told an urgent laser is the only path forward. Then we adjust the latch, slow the flow, and within days the pain drops and weight gain normalizes. That doesn’t mean releases are never helpful; it means timing and indication matter. The internet’s most persuasive stories are compelling precisely because they are personal, but personal stories don’t replace careful evaluation. A lip tie baby needs individualized, not ideological, care.
Do Lip Ties Cause Cavities, Speech Delays, or Orthodontic Issues?
You’ll hear claims that an untreated upper lip tie inevitably leads to cavities between the front teeth, gum recession, or speech issues later. The current scientific picture is more cautious. Dental hygiene habits, diet, saliva quality, and overall oral anatomy play stronger roles in caries risk than a frenulum alone.
Speech development is influenced by neuromuscular coordination, hearing, and environmental language exposure; a lip tie baby rarely needs an early procedure “to protect future speech.” As for spacing of the front teeth, the diastema in early childhood often closes naturally as the mouth grows and permanent teeth erupt. When future dental or speech concerns arise, we evaluate them on their own merits, not as automatic consequences of a newborn frenulum.
When a Procedure Might Help (and When I Recommend One)
After skilled lactation support and careful follow-up, some infants still struggle. When a lip tie baby also has signs of a functionally restrictive tongue tie—such as poor elevation, poor lateralization, and persistently shallow latch with objectively poor transfer—releasing the lingual frenulum can reduce maternal pain and sometimes improve feeding dynamics. The literature shows more consistent short-term nipple-pain relief from tongue-tie release than from isolated upper lip release. For an isolated lip tie with good tongue function, the benefits of procedure are less clear.
How I counsel families:
- Potential benefits. For select cases, a well-indicated release can reduce pain, allow a deeper latch, or improve transfer. If the lip tie baby has repeatedly failed conservative measures and function truly looks restricted, I will support a referral and coordinate care.
- Risks and trade-offs. Although complications are uncommon, we must discuss them: bleeding, infection, oral aversion, or simply no improvement—especially when the lip tie was not the primary cause. We also discuss the emotional and financial burden of procedures.
- Aftercare with common sense. I prefer gentle wound care and immediate return to feeding. I avoid aggressive stretching routines that may not help and can distress the baby. The goal is comfort and function, not elaborate exercises that interfere with bonding.
- Team approach. I collaborate with lactation consultants, pediatric dentists, and otolaryngologists I trust. A lip tie baby should not bounce between opinions; one coordinated plan avoids confusion and reduces stress.
Bottom line: I do recommend procedures when the pattern is clear, functionally restricted, and genuinely unresponsive to high-quality support. But I never promise a miracle, and I never rush a family.

Practical Feeding Strategies You Can Try Today
Whether you breastfeed, pump, or bottle feed, these steps often help a lip tie baby quickly:
- Laid-back positioning. Recline comfortably so gravity keeps baby deep on the breast. This can soften a fast let-down and improve latch depth.
- Deep, asymmetric latch. Tickle the upper lip and wait for the widest gape. Bring baby to you—belly to belly, nose opposite the nipple—aiming the nipple toward the palate. More areola should be in baby’s mouth below the nipple than above.
- Hand expression primer. Express a small amount before latching; it can coordinate let-down with baby’s suck, easing the first minute for a lip tie baby who struggles most at the start.
- Breast compressions. Gentle compressions during sucking bursts help sustain flow and keep the baby engaged without constant relatching.
- Paced bottle feeding. Hold the bottle more horizontal, pause every few sucks, and let baby “ask” for flow. Use a nipple with appropriate flow; too fast can cause coughing, too slow can frustrate.
- Skin-to-skin time. It improves feeding reflexes, regulates temperature and heart rate, and calms both parent and infant—crucial for a tense lip tie baby dyad.
- Track objective data. Diaper counts, weight checks, and a daily pain score. Clinical decisions for a lip tie baby should be anchored in numbers, not just impressions.
- Protect supply if needed. If milk transfer is low, add short, efficient pumping sessions after some feeds. A brief boost can carry the family through the learning period without undermining direct breastfeeding.
Real Clinic Stories (De-identified)
- Baby A, 2 weeks. Family was told to schedule an urgent upper lip laser after photos in a parenting group. In clinic, latch was shallow and let-down was fast. We used laid-back nursing and deep latch coaching. Maternal pain decreased from 7/10 to 2/10 in 48 hours; weight gain normalized. No procedure. Baby A is a classic lip tie baby whose problem was flow-management and latch depth, not the frenulum itself.
- Baby B, 3 weeks. Clear tongue elevation restriction, consistent transfer problems, and persistent maternal pain despite excellent technique and multiple consults. After a team discussion, Baby B underwent a carefully indicated lingual frenotomy. Post-procedure, latch improved and pain dropped. We did not release the upper lip because function no longer looked restricted. This lip tie baby had a real tongue-based problem; targeted treatment worked.
- Baby C, 6 weeks. Bottle-fed, gassy, clicking on higher-flow nipples. Switching to paced feeds with a slower nipple resolved the symptoms within days. The prominent upper frenulum remained, but the lip tie baby became comfortable and content.
These stories underline a single principle: treat the pattern, not the picture.
Addressing Common Myths About a Lip Tie Baby
Myth 1: “If you don’t fix it now, your child will have speech problems.”
Speech is multifactorial. A newborn’s upper labial frenulum rarely dictates future articulation. We monitor development and intervene if problems appear, not automatically at birth.
Myth 2: “All breastfeeding pain comes from ties.”
Not true. Positioning, latch depth, nipple shape, fast or slow flow, and early-weeks learning curves all contribute. A lip tie baby may be comfortable once these are optimized.
Myth 3: “Grades prove who needs surgery.”
Grades describe appearance. Function decides. Many high-graded frenula are asymptomatic; many low-graded ones are paired with other issues.
Myth 4: “Laser is always superior to scissors.”
When a procedure is indicated, outcomes depend more on indication, technique, aftercare, and follow-up than on the tool. The best approach is the one executed safely, for the right reasons, by an experienced clinician.
How I Communicate With Families (Compassion First)
The lip tie baby conversation can be emotional. Parents may feel guilty, pressured, or overwhelmed by conflicting advice. In my practice, I promise three things:
- No rushing. You will never be pushed into a procedure.
- Data and clarity. We decide using pain scores, weight trends, and observed function.
- Support regardless of path. Whether you choose expectant management, a procedure, pumping, or combination feeding, I remain on your team.
By centering the family’s values and the baby’s comfort, we consistently find the calmest, most effective plan for a lip tie baby.
A Simple Decision Framework You Can Use at Home
Ask these four questions over a week of intentional support:
- Is pain improving with optimized latch and positioning?
- Is weight gain appropriate for age?
- Is feeding becoming shorter, calmer, and more efficient?
- Does the upper lip evert comfortably during the latch when you’re in an ideal position?
If the answers trend “yes,” your lip tie baby may not need a procedure. If they remain “no” despite high-quality help, it’s reasonable to seek a coordinated evaluation for possible release—especially if tongue function looks restricted.
The Bottom Line (What I Tell Every Family)
- A visible upper frenulum is normal. The key is function, not photos.
- Most lip tie baby problems respond to skilled, hands-on feeding support.
- Procedures can help selected infants, especially with true tongue restriction that fails conservative care, but an isolated lip tie rarely demands urgent action.
- Let comfort, transfer, growth, and parental goals guide the plan.
- You deserve balanced counseling, gentle follow-up, and practical tools—not pressure.
As a physician, I’ve learned that the best outcomes for a lip tie baby happen when we blend evidence with empathy, watch a real feed, correct the simple things first, and reserve procedures for the few who truly need them. That approach protects babies, protects parents, and protects breastfeeding.
Final Encouragement
If you’re parenting a lip tie baby, you’re not alone. The first weeks are a crash course in anatomy, sleep deprivation, and strong opinions from every direction. Take a breath. Find a clinician and lactation consultant who will watch a full feed, who will speak plainly, and who will make a plan with you. With the right guidance, most families find comfort and confidence—often without a scalpel or a laser. And when a procedure is the right call, a calm, coordinated team can carry you through it safely and kindly.
Your lip tie baby deserves thoughtful care, and so do you.
Is this conversation helpful so far?